Educate. Empower. Support.
-
Patients want to feel involved in decisions about their treatment. We specialize in creating shared decision-making mobile apps that give patients a voice—a fully informed, meaningful voice—in the treatment planning conversation, and saves the healthcare team time during consultations. Patients can review relevant treatment information at their own pace, whenever and wherever is convenient for them. Informed, involved patients are happier, more compliant, and have better outcomes.
-
Whether you are a physician practice, specialist center, hospital, academic department, medical society, or in industry, we will design a shared decision-making app that addresses your specific patient education needs, branding and regulatory requirements, and saves providers time during consultations.
-
We offer top-quality, easy to use patient decision aids in the form of mobile apps, tailored to your needs, medical specialty and expertise—that run on an iPhone, iPad, and Android.
-
No other healthcare app company offers the high quality of Toliman at such an affordable price. We achieve this by using our successful shared decision-making technology to power all our apps. Using this proven, fully customizable framework “under the hood” means we don’t have to reinvent the wheel for your app, and you save many thousands of dollars in development costs.
-
Toliman offers the highest-quality shared decision-making mobile apps available anywhere.
-
We’ve already built a very successful interface and framework so customization is all that remains, making the overall process much faster than the normal development cycle for this type and quality of app.
- Proven Success
- Customized
- Functional
- Value
- Quality
- Speed
- Proven Success
- Customized
- Functional
- Value
- Quality
- Speed
Community

Knowledge Center

Decision Wizard

Community
Notice: Trying to access array offset on value of type null in /home/mfe7cxnrm557/public_html/tolimanhealth/wp-content/themes/toliman-theme/template-parts/proven-success.php on line 36
Knowledge Center
Notice: Trying to access array offset on value of type null in /home/mfe7cxnrm557/public_html/tolimanhealth/wp-content/themes/toliman-theme/template-parts/proven-success.php on line 60
Decision Wizard
Notice: Trying to access array offset on value of type null in /home/mfe7cxnrm557/public_html/tolimanhealth/wp-content/themes/toliman-theme/template-parts/proven-success.php on line 84

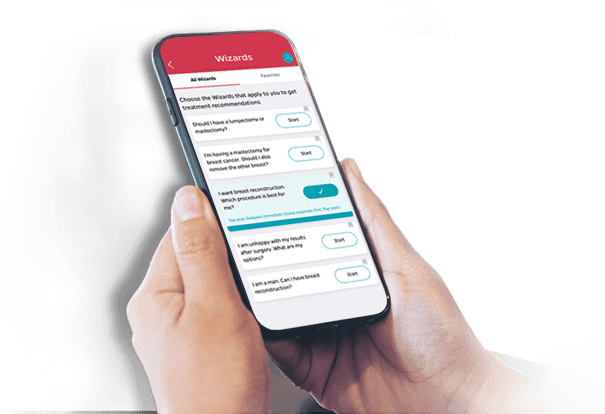
The Breast Advocate® App is the first shared decision-making app for breast cancer surgery and breast reconstruction. Breast Advocate® educates patients in a comprehensive and personalized way about ALL their breast cancer surgery and reconstruction options, provides access to the latest studies and expert opinions, and provides users much-needed support via it’s active community. Regardless of the patient’s diagnosis and situation, Breast Advocate® provides all the information and tools that patients need to take a more active role in their consultations and participate fully in the decisions about their treatment.
At Toliman, we use the same proven technology behind Breast Advocate® to power all our apps. Using our fully customizable framework “under the hood” will save you many thousands of dollars in development costs. All you need to focus on is how you want your new app to look, and the content you want to include. We will tailor your app to your needs, specialty, product, and branding, to facilitate both meaningful patient participation in the treatment decision-making process, and compliance with your regulatory requirements.
We can also create your own unique version of the Breast Advocate® App for your breast practice, breast center, academic institution, or patient advocacy organization… the same great concept, branded for you, and further customized with your own content. Please contact us for more information.
Best Apps for Managing Your Breast Cancer

Your phone is loaded with apps for finding the nearest gas station, keeping tabs on your kid’s soccer schedule, and locating an Uber to the airport. But should you trust an app to manage your breast cancer? Short answer: Yes. Downloading one can help you organize your breast cancer treatment and ease the stress that accompanies diagnosis, according to a study at the University of Amsterdam, something that your doctor should support. “Your doctor should be positive about you taking the initiative with your health,” says lead author Chiara Jongerius. The big question: Which app to use? We’re very proud to report that our flagship shared decision-making app, Breast Advocate® is one of them!
Read MoreThe Best 5 Apps to Support Breast Cancer Patients

One in eight US women develop breast cancer over the course of their lifetime, making it the second most common cancer in American women. The journey is never easy, but there are many steps you can take to support yourself or a friend with breast cancer.
Being more educated about a health complication, acquiring methods to track it, having the means to get your questions answered, and receiving mental support are all important measures one can take.
There are many apps out there that are specifically designed to serve this purpose. We’re very proud to report that our flagship app, Breast Advocate® made this exclusive list!
Read MoreShared Decision Making: Putting The Patient at the Center of Healthcare

By explicitly recognizing a patient’s right to make decisions about their care, shared decision making can help ensure that care is truly patient-centered.
As gravity shifts away from health care providers as the sole keeper of medical information, the importance of sharing decisions, as opposed to clinicians making decisions on behalf of patients, has been increasingly recognized.
Shared decision-making (SDM) is the conversation that happens between a patient and clinician to reach a healthcare choice together.
Read MoreThe Importance of Shared Decision-Making

When planning any type of medical treatment, interactions between the patient and their clinical care team tend to fall into one of the following types: paternalistic, informative, or shared decision-making.
Paternalistic decision-making occurs when the physician decides which course of action or treatment is in the patient’s best interest, without involving the patient in the decision-making process, i.e., “Here’s what we’re going to do for you Mrs. Smith.”
The “Informative” approach to decision-making provides the patient more comprehensive information including pros and cons, and the risk of complications, but still does not consider the patient’s values or preferences.
Shared decision-making occurs when the health care provider and patient work together to make a health care decision that is best for the patient. The optimal decision takes into account…
Read MoreShared Decision-Making: Improves care while lowering costs

A report published in the New England Journal of Medicine touts that shared decision-making provides many benefits for patients, clinicians, and the healthcare system as a whole. These benefits include improved patient knowledge, less anxiety over the care process, improved health outcomes, reductions in unwarranted variation in care and costs, and better alignment of care with patients’ values.
Even the Affordable Care Act (ACA) thinks so. It has a provision in it that encourages greater use of shared decision-making in health care.
Patients and their families often get confused and overwhelmed when making complex medical decisions where there is more than one treatment option. Shared decision-making, a collaborative process between patients and their physicians, can help clear up questions efficiently and better aligns patients’ preferences and values with treatment plans.
Decision aids
One key to shared decision making is using patient decision aids…
Read MoreWhy Value-Based Care Must Include Shared Decision-Making

Shared decision-making is a key patient engagement strategy, but not yet widespread. Healthcare professionals say integrating the practice into value-based care could spark adoption.
Shared decision-making, or the practice of an informed patient participating in treatment decisions alongside her clinicians, may seem like a natural patient engagement strategy. After all, shared decision-making integrates the patient into the healthcare process and gives the patient more claim in her wellness journey.
Shared decision-making has shown to reduce preventable hospital readmissions among cardiac patients by at least 19 percent, and can also decrease patient anxiety and healthcare costs.
But despite proven clinical efficacy, shared decision-making isn’t entirely widespread across the healthcare industry, says Peter Goldbach, MD, Chief Medical Officer for Rite Aid’s RediClinic and Health Dialog…
Read More




